Our Research

The Laboratory of Translational Psychiatry combines animal models and human data to understand the neurobiology of psychiatric disorders. We aim to develop new treatments for patients by uncovering the molecular underpinnings of mental illness. Our research focuses on neuroimmune interactions and the role of the gut microbiome in substance use disorders, neurodegenerative disease, depression, and autism. By investigating these complex interactions, we hope to unlock new therapeutic possibilities for improving mental health.
What We Study
conditions

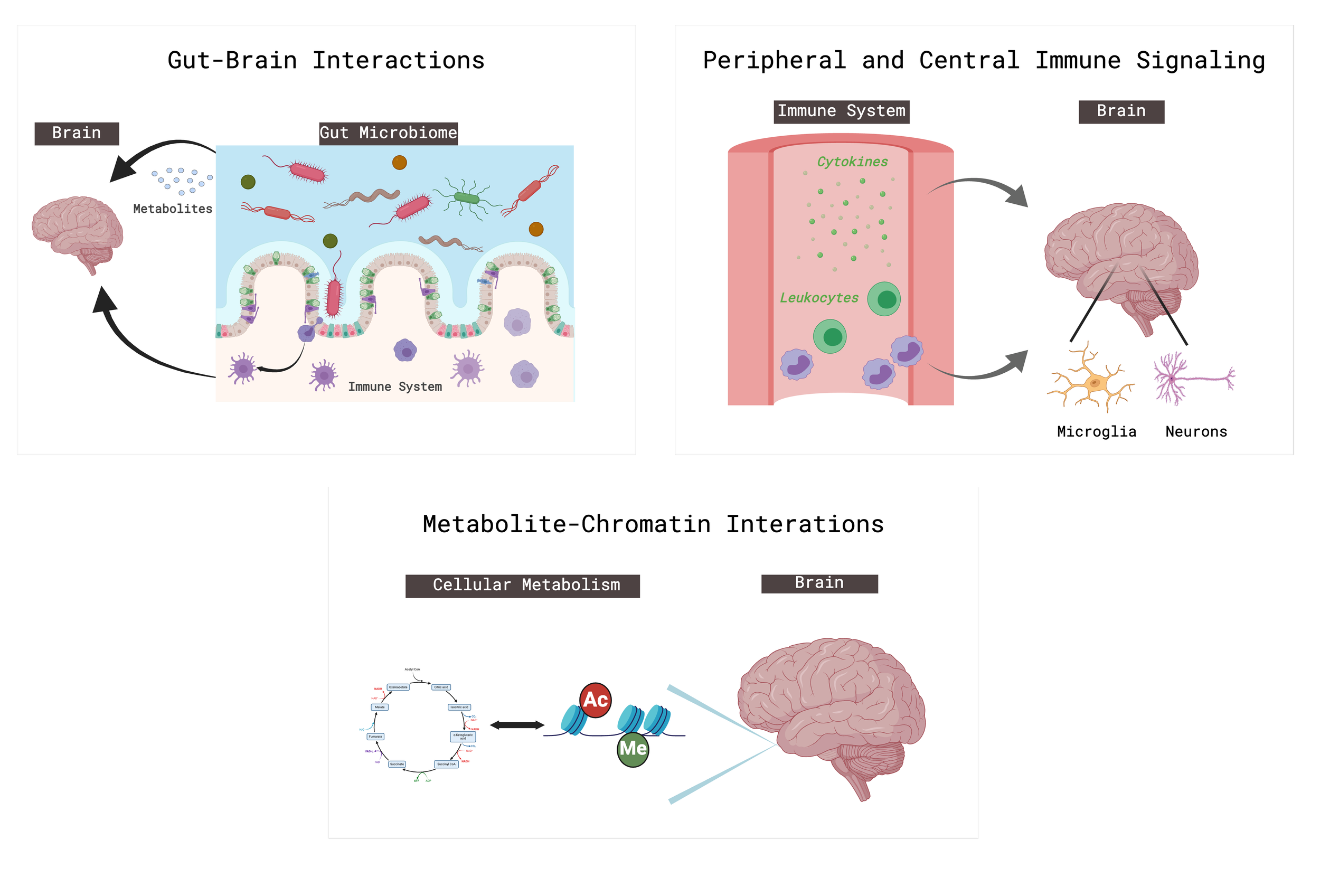
mechanisms
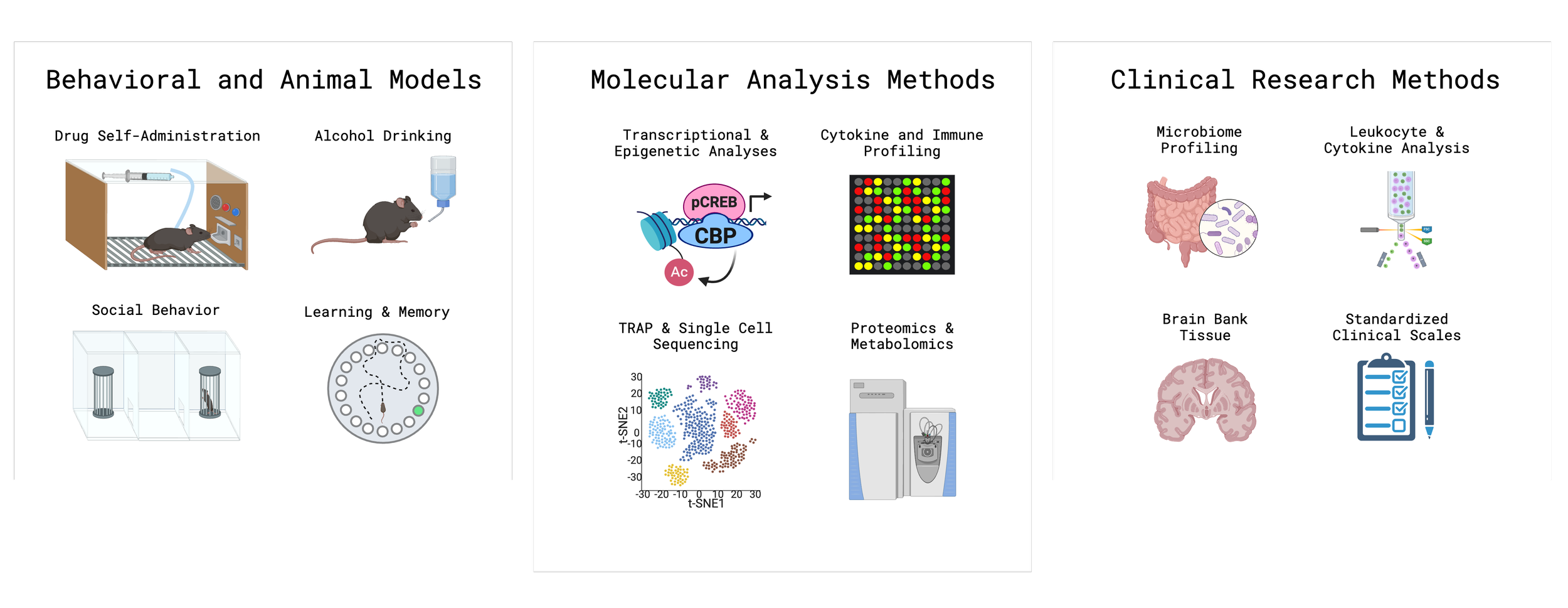
methods